Benlysta, A New Treatment for Lupus
Lupus, an autoimmune disease, turned up on the front page, right side of today’s Wall Street Journal. It cropped up, also, on the first page of the New York Times business section, and elsewhere. Scientific American published a nice on-line review, just now. The reason is that yesterday the FDA approved a new, monoclonal antibody for treatment of this condition.
The drug, Benlysta (belimumab), targets a molecule called BlyS (B-lymphocyte Stimulator). The newspapers uniformly emphasize that this drug marks some sort of triumph for Human Genome Sciences, a biotech company that first reported on BlyS in the journal Science way back in 1999. BlyS triggers B cells to produce antibodies that, in patients with lupus tend to bind and destroy their own cells’ needed machinery, causing various joint, lung, liver, kidney, brain, blood vessel and other sometimes life-threatening problems. So if and when Benlysta works, it probably does so by blocking aberrant, autoimmune B cell activity.
The papers don’t give a lot of details on the drug’s effectiveness, except that it appears to help roughly 1 in 11 patients and the main benefit may be that some lupus patients on Benlysta can reduce their use of steroids, which have long-term and toxic effects on many organs. The most recent, major medical publication on a trial on the drug came out in the Lancet, two weeks ago.
Some reported caveats are that the drug has not been adequately tested or approved for patients with severe kidney or neurological manifestations of the disease, and that its activity, marginal as it is, appears to be less in patients of African heritage based on trials completed thus far. Additional trials are in the works.
The drug is expensive, to the updated tune of $35,000 per year. According to the WSJ: “Estimates of how many Americans are affected range from 161,000 to 1.5 million.” (How’s that for a wide ballpark figure? – likely a function of how hard it is to define and establish diagnosis for this disease, which anticipates how hard it will be to measure this drug’s effects, see below.) The same Journal piece says analysts expect the drug to become a blockbuster, with annual sales eventually topping $1 billion.
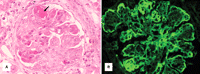
I’ve been intrigued by lupus ever since I was a second-year medical student, studying pathology before BlyS was discovered and monoclonal antibodies could be bulk-manufactured and tested in clinical trials. The disease’s name – from the Latin term for wolf, refers to the appearance of a facial rash that some patients develop.
Lupus can be scary to treat. One of my clearest late-night memories of my residency was when a 23 year old woman with lupus “rolled in,” as we would say, to the E.R. around 5:30 AM, as I was nearing the end of my then nearly-unrestricted shift. “We’ve got a sickie,” a nurse said as she roused me from my work on a hand-written note about someone else. The patient was dehydrated and gasping for air, and I remember having trouble getting her IV in, but somehow I did and she made it at least to the ICU.
From an immunologist’s perspective, it’s a fascinating condition because it flares and quiets – sometimes on its own – and affects different organs in distinct patterns among patients. The causes of lupus are likely varied. It may be that shutting down BlyS with an antibody is just a fancy and possibly more-targeted, less-toxic way of doing what steroids, like prednisone, do to B lymphocytes.
The problem I’d anticipate with the trials – carried out by my ever-patient, expert rheumatology colleagues – is that it’s sometimes hard to measure disease activity and responsiveness in lupus, apart from the kidney, because so many of the symptoms are subjective. And because the disease can affect so many organs, it’ll be hard to appreciate the drug’s toxicity, as apart from disease in itself.
—
Leave a Reply