Perspective on Screening for Sickle Cell Trait in Student Athletes
Today I watched a video, The Student-Athlete with the Sickle Cell Trait, sponsored by the National Collegiate Athletic Association (NCAA) on its website. The 12-minute presentation provides some helpful background on what it means to have sickle cell trait and how awareness of that condition might influence a student’s (or coach’s?) behavior during rigorous conditioning and competitive sports.
“The more medical information we know about our student athletes, the better equipped we are to help keep them safe,” says Mark Richt, Head Coach at the University of Georgia, at around 3 minutes into the clip.
A new NCAA policy mandates screening all Division I college sports participants for sickle cell trait. Not coincidentally, the Sept 9 issue of the New England Journal of Medicine opens with a noteworthy perspective* on this topic. The screening recommendation, effective at the start of this academic year (i.e. now) directly affects more than a few young adults in the U.S.: among nearly 170,000 athletes who’ll be tested this year, it’s expected that several hundred “carriers” will be identified.
The issue, as considered by the group from the NIH and Johns Hopkins University who authored the NEJM paper, draws on some fairly old hematology – on genetic aspects of sickle cell anemia, a disorder of hemoglobin synthesis, and on clinical features of having just the trait – in the context of public health and the current controversy on direct-to-consumer DNA testing.
Some background:
Sickle cell trait is, usually, an asymptomatic condition. Having the “trait” refers to a carrier state – when a person inherits one abnormal gene that would cause disease if both were affected. It’s a common condition, present in more than 2 million people in the U.S. While the prevalence of sickle cell trait is highest among people of African decent (at a rate approaching 8 percent), it does occur in other groups including Hispanics and whites.
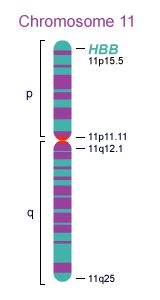
The sickle cell variant, or mutation, is located in the gene encoding beta hemoglobin on human chromosome 11. For a person to develop disease the mutation needs to be present on each of two genes, on the relevant chromosomes inherited from each parent, in what’s called a homozygous state.
Hemoglobin is a complex protein in red blood cells that plays a critical role in binding oxygen and delivering it throughout the body to tissues where it’s needed – including the brain, lungs, heart, kidneys and muscles. In healthy human adults, the most common form of hemoglobin in blood cells is a large molecule called hemoglobin A.
What happens in people who inherit the sickle cell mutation – a single nucleotide polymorphism, or “SNP” in modern jargon – is that the altered DNA sequence yields an abnormal beta globin chain. The resultant protein contains an amino acid switch: a valine instead of a glutamic acid residue at position 6. This seemingly small, single amino-acid difference in the beta chain structure can wreak havoc by changing the molecule’s electrical charge and solubility.
Clinical picture for sickle cell trait:
In approximately 40 states in the U.S., newborn babies are screened for sickle cell anemia and trait. Still, many adult carriers are unaware of their status.
For the most part, having sickle cell trait doesn’t cause illness. It doesn’t, in itself, cause anemia or shorten a person’s life expectancy. That’s because in the heterozygous condition there’s usually enough hemoglobin A to take care of the body’s oxygen-delivery needs. Still, there have been some, occasional reports of complications and rare episodes of sudden death.
Patients with sickle cell trait are, just slightly, prone to problems with the kidneys, spleen, and, rarely, rhabdomyolysis – a condition in which the muscles break down rapidly under stress and low oxygen, leading to kidney damage and, ultimately, irregular heart beats. The risk for this potentially lethal syndrome is elevated during heat exposure, dehydration and intense physical exertion.
Perspective on the screening program:
In 2006, a 19-year-old freshman player at Rice University collapsed on the field at football practice. His death, attributed to rhabdomyolysis in the context of sickle cell trait, might have been avoided had the student and his coach taken precautions. It’s for this reason that the NCAA has advocated screening of all student athletes for this condition.
The idea is to avoid preventable deaths by knowing more about the athletes’ disposition to exertional rhabdomyolysis before it happens, by screening the entire group of players for sickle cell trait. In some ways this seems like a pro-active, well-intentioned policy that could save lives.
On the other hand, as discussed in the NEJM piece*, the new screening policy raises a host of challenging issues:
- how will colleges inform minor players’ parents about results?
- how will the schools handle players’ privacy?
- might athletic scholarships be contingent on blood-test reports?
- what’s to be done about college athletes who don’t play in Division I? (should we test all college students for sickle cell trait? what about high school students? should we screen for other medical conditions, while we’re at it? – because we could…)
- how will the schools manage communication and questions regarding the test findings? (for the most part, the program is run outside of doctors’ offices)
- what about false positives and other testing errors that might arise? (even if the percent of errors is quite low, if you’re testing 170,000 students, there might be an accidentally switched-sample or two)
- and more – could the test results lead to discrimination, such as in post-college employment in professional sports?
A field day of questions!
What’s noteworthy, also, is the relevance to the current debate on genetic testing of seemingly health people for all sorts of conditions, like cystic fibrosis, hemochromatosis and other measurable traits. There’s a parallel suggestion here, that perhaps most of the behavioral changes people would make upon finding they’re a carrier for a particular condition would be universally advisable, regardless of the test results:
Key questions for the NCAA are whether equivalent interventions can reduce risk in student athletes with sickle cell trait and whether changing the practice and culture of college athletics by instituting prevention measures for everyone would be more beneficial than targeted interventions….
And toward the NEJM paper’s conclusion:
… there is now great interest in genetic-based risk profiling and personalized medicine. Although the NCAA program shares some elements with these new approaches to care, it differs from them in many ways: the screening takes place outside the physician–patient relationship, the “patient” is undergoing testing because his or her genetic makeup may produce an adverse reaction in circumstances related to a chosen avocation, and the possible corrective “intervention” — modification of practice and training regimens — could require a shift in the culture of sports.
This is a long post on a complex topic that still needs more attention.
What strikes me is that sickle cell anemia is a tough disease but it was one of the first described and is relatively simple in its molecular underpinnings. Most illnesses and malignancies are multi-factorial; many involve multiple genetic hits in genes for less familiar signaling molecules and enzymes. I can’t really see how doctors or coaches or doctors or public health officials will inform the public about their genetic and other screening results, in a meaningful way, without better all-around education in the U.S.
And this – sickle cell trait – is just one of hundreds of examples of heritable conditions for which we might test, soon. If a high school graduate doesn’t know what an amino acid is, or DNA or hemoglobin, it’s hard to have these discussions. The gap between what scientists understand, doctors study and might explain, and the public discourse on the same, is mind-boggling.
….
*subscription required
O have a 13 year old son with the sickle cell trait. He has severe ADHD which keeps him over active most of his days. I want to know if there should be more indepth testing due to the trait with his chronic migraines, muscle aches, now he is passing out at times, all of my children have “iron deficent” anemia and they take extra iron and eat more green leafy veggies, liver is out of the question, but continue to read with low iron.He has a different father and his father carried the trait. I just wanted to know if these symptoms are worth looking at as a cause of the trait. He also is now dx with asthma and had chest pain, cant stand to be hot? will not even swim in the pool if its too hot outside, Please respond.
Hi Kari,
I can’t provide medical advice on this blog. Most but not all people with sickle cell trait have no symptoms. It sounds like you should take your son to the pediatrician or family doctor, so that he can be properly evaluated.