Swedish Mammography Report Finds Benefit In Screening Younger Women
I’m not sure why editors buried last week’s report on the new Swedish mammography study. The positive findings appeared only on page 24 of Thursday’s (Sept. 30) print edition of the New York Times. My husband didn’t hear about it on NPR on his way home from work. The moms in my community didn’t see Dr. Gupta talking about this on TV.
The new findings – linking mammograms for women aged 40 to 49 to a big drop in BC death rates years later – seem to confound journalists’ notions on screening’s lack of effectiveness in this disease. But they’re no surprise to doctors like oncologists who have experience caring for breast cancer patients.
The Swedish study, with lead and senior authors in the Department of Radiation Sciences at an oncology center at Umeå University in Sweden, was presented at an annual ASCO* breast cancer symposium and published on-line** last week in the ACS journal Cancer. The data reveal that for women living in Sweden where mammography was offered every 18 or 24 months to women ages 40 to 49, breast cancer-related deaths fell by approximately 26 percent.
In some ways, the new report is similar to a highly-publicized paper published a week earlier in the NEJM: both are based on historical data, between 1986 until 2005, extracted from comprehensive, public databases in a Scandinavian nation. What’s different here, besides the positive results and younger age group focus, is that follow-up was much longer in this Swedish study: 16 years after a BC diagnosis; it was a measly 2.2 years in the Norway study.
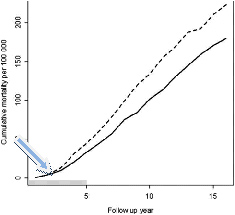
This graph to the right, adapted from Figure 2 in the original Swedish report, shows the crude cumulative breast cancer mortality per 100,000 person-years. The solid line shows survival for women found to have BC in the study group – those women living in areas where mammography was provided between ages 40 and 49; the dashed line shows the same for the controls – those living in areas where women between 40 and 49 years “were not invited to attend” service (i.e. government-financed) screening.
The light blue arrow, which I’ve added, points toward the 2.2 year mark, the average follow-up for patients in the recent Norway study. What’s evident is that such a short interval is not nearly sufficient – it’s far too early – to assess the effects of mammography on mortality in women with BC; over years, the divergent curves show a marked benefit of screening.
As an oncologist, I know this finding meshes with reality; breast cancer tends to kill women years, rather than months, after the time of initial diagnosis; you wouldn’t expect mammography to make a dent in a mortality curve until after 4-5 years or so, especially if you factor in possible lead-time bias, as the Swedish study authors did.
Some legitimate concerns about the Swedish study include that it comes from a radiology group with an “interest” in having mammography be effective. Let’s say that’s true, but it also may be that those physicians become breast cancer researchers with good intentions, and that mammography does save lives by catching early-stage BC. It would be foolish to deny that radiologists, oncologists and others in the field have the most experience with breast cancer imaging, diagnosis and treatment.
This positive report should be scrutinized, yes, but no more or less than the other papers on the same subject that have been highlighted, selectively, in the media. How journalists cover mammography studies, and that they do so with an open mind, matters a lot.
—
*disclosure: I am an ASCO member.
**full-text by subscription
***Hellquist, B. N., Duffy, S. W., Abdsaleh, S., Björneld, L., Bordás, P., Tabár, L., Viták, B., Zackrisson, S., Nyström, L. and Jonsson, H., “Effectiveness of population-based service screening with mammography for women ages 40 to 49 years,” Cancer, 2010, Volume and pages pending (on-line only, citation in progress)
Leave a Reply